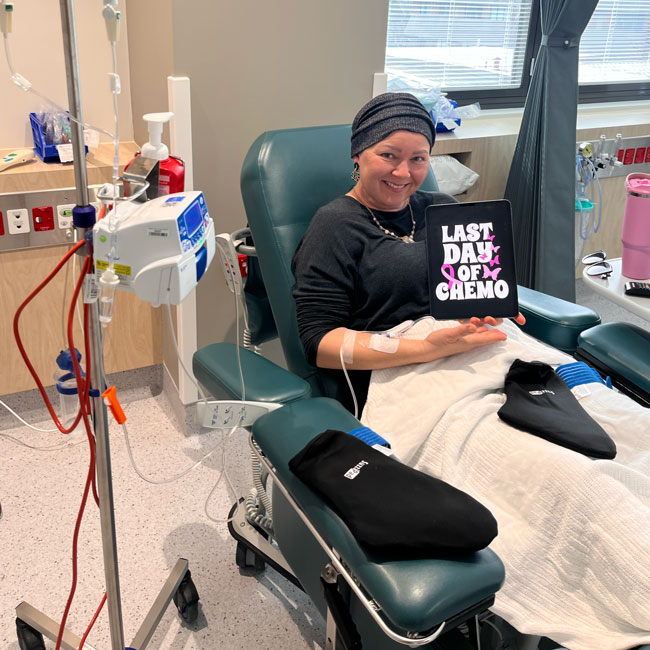
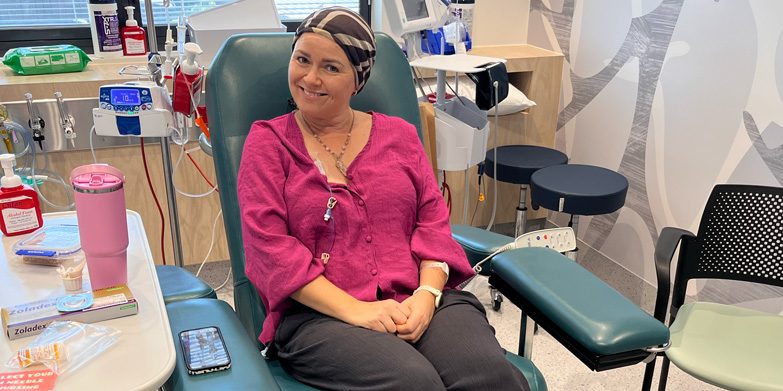
When Rachel, Founder of North Shore Mums, began chemotherapy for breast cancer, she was terrified and overwhelmed by the unknowns ahead. Now, having completed five months of treatment, she shares her personal journey and practical tips to help others navigate the physical and emotional challenges with a sense of hope and resilience.
I’ve just completed five months of chemotherapy. Before starting the treatment, I was utterly terrified, overwhelmed by the possible side effects and the unknown toll it might take on my body.
At my first appointment with the Medical Oncologist, she talked me through the treatment plan and the list of potential side effects. Some, like hair loss, were a given. Others varied from person to person. While it’s essential to be fully informed, hearing it all at once was overwhelming — I spent much of the appointment in tears. But despite the fear, I was determined to complete the treatment and face any side effects, so I could maximise my chances of being here for many years to come.
From the beginning, I was determined to support my body in every way I could—to ease the side effects and give myself the best possible chance of keeping the cancer from coming back.
My chemotherapy experience wasn’t nearly as awful as I feared. Although some days were a struggle, most were manageable. I managed to lead a relatively normal life (to go to the supermarket, meet friends for lunch in a cafe, watch my kids play sports, attend dance concerts and school musicals), and I didn’t get sick (even when my kids came home with viruses!).
Now that I’m on the other side of chemo, I want to share what helped me in the hope it might support others who are just starting this journey.
Please keep in mind, I’m not a medical professional. I’m simply a breast cancer patient who did everything I could to care for my body, mind, and spirit throughout treatment—and I hope that by sharing my personal experience, it gives other people hope and ideas to support their body, too.
My Chemotherapy Treatment
Before my diagnosis, I thought chemo was chemo. I had no idea there were so many different types of chemotherapy drugs, with different combinations and regimens for various cancers and outcomes.
My treatment was to run for five months, starting with four fortnightly cycles of AC Chemotherapy, followed by 12 weekly cycles of Paclitaxol.
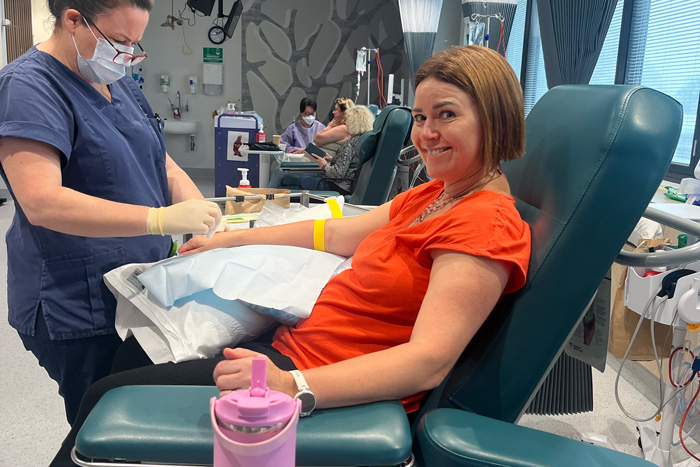
A nervous smile before Rachel’s first chemo infusion in January 2025
AC Chemotherapy
AC Chemotherapy involves the use of two drugs: doxorubicin (the ‘red devil’) and cyclophosphamide. As far as chemotherapy goes, this particular drug is strong and considered about a ‘9 out of 10’ in severity of side effects.
Hair Loss
I won’t sugarcoat it. Losing my hair was probably the most confronting aspect of chemotherapy. I’ve had the same hairstyle (brown, shoulder-length) for years and have never experimented with different styles. So I’ve been used to seeing the same person in the mirror!
About a month before starting chemo, I cut my hair to a short bob (from shoulder length). I did this to get accustomed to a different look and so that I’d have less hair falling out when the time came.
Exactly two weeks after my first AC infusion, my hair started falling out. It happened very quickly. One day, I was brushing my hair as usual, and the next day, it came out in clumps as I washed it in the shower. Even though I knew it was coming, I was shocked. The hair kept falling out. On my pillow, on my clothes, in the shower. It was very distressing.
View this post on Instagram
A post shared by North Shore Mum with Breast Cancer (@northshoremum.breastcancer)
After a few days, I decided to ‘take control’, so I visited a lovely local hairdresser with a home salon for a pixie cut. She was incredibly caring and compassionate about my situation, and I am so grateful that I could do it in the privacy of her salon with only my family looking on.
Although everyone politely said it looked “great,” I didn’t like it at all. It just wasn’t a style I would have chosen for myself!
Even with the pixie cut, chunks of hair continued to fall out, so I returned to her the very next day for a ‘number two’.
I’ll be honest. I’ve not embraced the bald head. Some women like to ‘rock it,’ and I have so much respect for people with that kind of confidence! I’ve spent a small fortune experimenting with various head coverings, hats, and the occasional wig. My head is mostly covered, even when I’m at home.
Sleep
Sleeping is vital for recovery, yet staying asleep during the night was my biggest challenge on this treatment.
With AC chemotherapy, you’re given steroids to take for the first few days after the infusion (to manage side effects and enhance the chemotherapy’s effectiveness by reducing inflammation, nausea, vomiting, and allergic reactions). Steroids should be taken first thing in the morning (as you get quite ‘wired!’), but they still considerably impacted my sleep.
I often woke up at 2 a.m. and couldn’t get back to sleep. Of course, a lack of sleep has a knock-on effect on my overall well-being during the day. I knew how vital sleep is to recovery, yet I struggled with it.
Although decent sleep didn’t come until I finished the AC chemo, the following helped:
- Journaling – writing down my thoughts before going to sleep. Getting them out of my head and onto paper was helpful.
- Supplements – DFH TriMag Supreme Night and Melatonin before bed
- Sleeping pill – after mentioning my sleep issues to my oncologist, she prescribed me a sleeping pill, which I took on the first few days of the cycle.
- Kindle – reading was a good distraction and took my mind off my darker thoughts.
- Calm – I listened to sleep stories, soundscapes, and meditations on my Calm app. Try Calm for FREE for 30 days.
Nausea
The chemotherapy nurse will give you anti-nausea medication as a precaution. I mainly experienced nausea in the first few days after the AC infusion, but ensured I took the pills before it had the opportunity to escalate. It wasn’t as bad as morning sickness or a self-induced hangover!
Altered taste in the mouth
By the third and fourth cycles of AC, my mouth had developed a few ulcers, and my tongue had become very white. Everything tasted like soap! Chemotherapy drugs can alter the taste receptors in the mouth, leading to distorted taste perceptions. Eating was no longer pleasurable, but I persisted as I knew how important good nutrition was for my recovery.
Paclitaxel
Compared to AC, paclitaxel was a breeze. I started sleeping better, could tolerate all food, and began to feel more like myself.
Neuropathy
One of the most serious side effects of Paclitaxel is peripheral neuropathy – numbness and tingling in the fingers and toes.
To reduce the risk of this happening, I decided to try ice gloves and socks. I’d heard that it had a reasonable success rate, and I found some on Amazon for just $85. No harm in trying!
The idea is that keeping hands and feet cold during chemotherapy may reduce blood flow to those areas, potentially limiting the amount of chemotherapy drug that reaches the nerves and causes damage. This involved freezing ice packs and slipping them into the gloves and socks, and wearing them throughout the infusion. Although it was slightly uncomfortable and meant I couldn’t use my hands or fingers during treatment, it was worth the inconvenience, as I didn’t develop peripheral neuropathy.
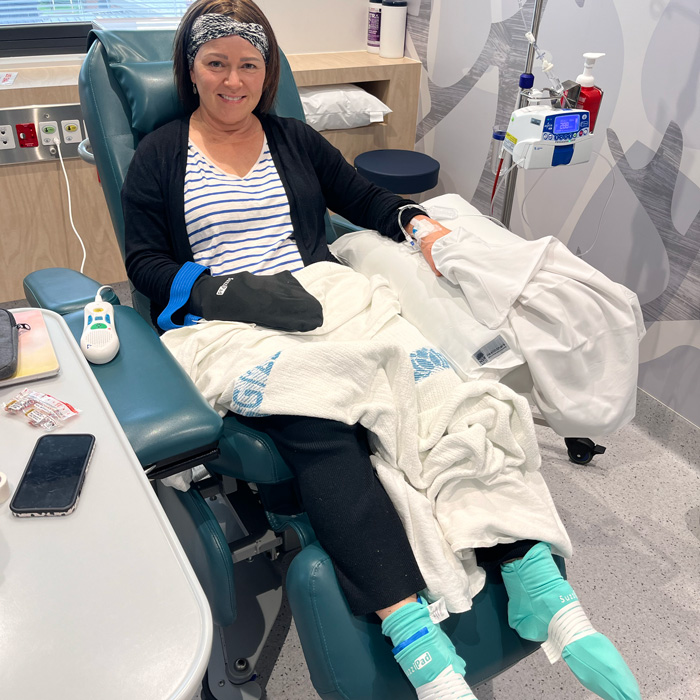
Ice gloves and socks to reduce peripheral neuropathy
Edema (Water Retention)
By about the 10th paclitaxel infusion, I developed edema (water retention). Some mornings, I’d wake up and find a big pocket of fluid above my eyelid and puffy bags beneath, and my face would be puffy. I’d also find indents where my socks were on my legs or the watch on my wrist. Edema is a side effect of Taxol, and it only occurred for me in the last few infusions, although it persisted for about a month after treatment completion.
It was explained to me that my kidneys and liver were working hard to eliminate other toxins, so the water retention was lower on the list of body priorities. I found some beneficial ‘face yoga’ videos on YouTube, and also had some lymphatic massage. I also tried to drink plenty of water and ensure I exercised every day. Ultimately, it’s just a matter of time before your body can clear the system.
Tips to get through chemotherapy
As well as dealing with the specific side effects listed above, I did a range of other things to support my body through chemotherapy.
1. Keep active
I’ve always exercised regularly, but sticking with my usual 5:30 a.m. outdoor training sessions felt too brutal during chemotherapy. I wanted to allow myself to rest, sleep in without an alarm clock, and find something more gentle that I could easily work into my day. For me, that was walking.
Walking is one of the most accessible and beneficial forms of exercise during chemotherapy, and it made a real difference.
Instead of my regular workouts, I walked 45 to 60 minutes daily.
- It lifted my mood. Physical activity releases endorphins and helps regulate emotions — something I needed while navigating the emotional ups and downs of treatment. Even on the darkest days, I forced myself out the door, and I always felt better afterwards.
- It helped ease side effects. Just 10 to 20 minutes of walking can improve circulation, boost oxygen flow, and support energy metabolism. It made my body feel more efficient — like it worked with me instead of against me.
- It gave me more energy. It seems counterintuitive, but gentle movement, such as walking, energises the body, helping to break the chemo-fatigue cycle that can be debilitating.
- It helped me manage my weight. Weight gain is typical during chemotherapy (though some people also lose weight). I was pleased to maintain my weight throughout treatment — no extra kilos. While I still aim to lower my BMI, avoiding weight gain during chemo felt like a small win.
Chemo fatigue can feel overwhelming, but walking helped me regain some strength, routine, and sanity.
2. Drink lots of water
Staying hydrated is essential during chemotherapy. Drinking plenty of water helps your body flush out the chemo drugs more efficiently, reducing side effects and supporting recovery. I made a conscious effort to drink lots of water, especially the day before, the day of, and several days after each treatment. I’m talking at least 3 to 4 litres a day.
I always had a water bottle with me — whether at my desk, in the car, by my bedside, or heading out the door. To make it more enjoyable, I’d often add a splash of lemon for a little extra flavour.
I also invested in a six-stage reverse osmosis water filter for our kitchen. After learning more about what’s actually in Sydney tap water, I wanted to ensure I was putting the cleanest, purest water into my body, especially during such a vulnerable time. Our filtered water is now free from contaminants and infused with beneficial minerals, giving me peace of mind whenever I fill my glass.
3. Eat a nutritious diet
Food is medicine! Eating a nutritious, balanced diet was one of the most powerful ways I supported my body during treatment. But honestly? It was overwhelming at first. There’s so much conflicting information online about what you should or shouldn’t eat when you have cancer. I felt completely confused.
Ultimately, I decided to see a qualified nutritionist specialising in oncology. That was a game-changer. Together, we determined the optimal approach for my body — one that supports my immune system, energy levels, and recovery.
For me, that meant focusing on:
- Plenty of fibre
- High-quality protein
- Lots of vegetables, especially leafy greens
- Legumes and lentils
- Small amounts of lean meat
I also found incredible guidance from Dr William Li — a doctor, scientist, and author of Eat to Beat Disease and Food Is Medicine. He shares evidence-based insights on how certain foods can help the body fight cancer and prevent its return. Inspired by his research, I added more foods to my diet, like:
- Berries (blueberries, strawberries, raspberries, blackberries) – berries are packed with polyphenols and antioxidants
- Green Tea (and Matcha) – rich in catechins like EGCG, anti-inflammatory and supports immune function
- Cruciferous Vegetables (broccoli, cauliflower, kale, brussel sprouts)
- Tomatoes – high in lycopene, especially when cooked
- Fatty Fish (salmon, sardines) – rich in omega-3 fatty acids
- Dark Chocolate (in moderation) – choose one that is high in cocoa (70% or more), low in sugar, and preferably organic.
- Nuts & Seeds (walnuts, flaxseeds, chia) – contain healthy fats, fibre, and anti-inflammatory compounds
- Pomegranate – high in ellagic acid and polyphenols
- Leafy Greens (spinach, watercress)
- Soy milk (yes, soy milk is safe and may also be beneficial for oestrogen-positive breast cancer).
What food should you avoid to lower your cancer risk?
- Processed meats – these have been linked to increased cancer risk, so steer clear of processed meat like bacon, ham, salami, sausages and chorizo
- Processed and ultra-processed foods – Whole foods are best! Ultra-processed foods often contain artificial preservatives, colours, flavours, emulsifiers, and sweeteners — chemicals your body doesn’t recognise or need. Some of these additives may disrupt gut health or increase inflammation, which can affect immune function and potentially increase the risk of cancer.
4. Don’t drink alcohol
Your liver is already working hard to process the effects of chemotherapy, so adding alcohol into the mix only increases the strain. There’s also strong evidence linking alcohol to a higher risk of developing many types of cancer, particularly breast cancer, and even more so for hormone-positive types.
I stopped drinking the moment I was diagnosed. And the more I learn about alcohol’s role in increasing the risk of recurrence, the more certain I am that I may never drink again.
“For women who have had breast cancer, alcohol consumption can affect the risk of cancer returning. Drinking alcohol raises oestrogen levels, which can fuel the growth of oestrogen-sensitive breast cancers. This can increase the chances of recurrence, particularly for women in remission or those with hormone-receptor positive cancers.” – Breast Cancer Trials
5. Get extra support for your body with Allied & Holistic Health
I was determined to look at other ways to support my body through chemotherapy, so I used a range of other health practitioners:
Lifestyle Medicine – I did a 12-week Breast Cancer program at The ELIA Lifestyle Clinic at The San in Wahroonga. This program included appointments with an interdisciplinary team consisting of an Integrative GP, registered nurses, health coaches, an exercise physiologist and a dietitian. This was invaluable in teaching me additional things I could do to support my body.
Naturopath – I found an amazing Naturopath, Carla Wrenn, who has a special interest in Integrative Oncology. She is very well respected in the cancer space and was recommended to me by several people. After a one-hour Zoom consultation (she is based in the Mornington Peninsula), she prescribed me a range of supplements to support my body. Before buying them, I showed the list to my Oncologist, who was happy for me to proceed. Hand on heart, I believe that these supplements helped reduce my side effects.
Lymphodema Physiotherapist – Although not directly related to the chemotherapy, I’m regularly seeing a Lymphodema Physiotherapist to help reduce the risk of developing lymphedema in my left arm, as all the lymph nodes in my armpit were removed during surgery
Chiropractor – I wanted to give my body the best chance to stay strong and resilient, so I opted for chiropractic care during my treatment. Chiropractic adjustments can support the immune system, reduce stress, and keep inflammation in check.
6. Reduce the stress in your life
Like every mum, life is hectic. But I tried to reduce the stress in my life. It’s still a work in progress – juggling the calendars of three children and running a business full time.
Accept Help – Accept help from any friends or family who have offered to deliver meals, run your children around, or perform other random acts of kindness. This is the time to accept help and know that one day, you can forward that help to other friends in crisis.
Say ‘no’ – This is also a time to say “no” to things you don’t want to do.
Give yourself time to rest – Put your feet up. Have a nap in the afternoon. Watch Netflix during the day. Learn to meditate. Try tapping. Try breathwork!
7. Share all your side effects and questions with your Oncologist & Nurses
Keep a note of any side effects you experience or any questions you might have, so you don’t forget anything when you meet with your Oncologist or Chemotherapy Nurse. It’s vital they know exactly what’s going on for you, and they can also prescribe specific medication or recommend products to ease side effects.
8. Look Good, Feel Better
There’s some truth to the notion that if you look good, you feel better. If you need a little inspiration, the Look Good, Feel Better Workshops are specifically designed for people with any type of cancer to help manage the most common physical and psychological impacts of treatment. I joined a 2-hour free workshop at The San in Wahroonga, and had a fun morning with other ladies facing image challenges since their diagnosis.
In a comfortable and supportive group environment, our dedicated team of volunteers address common concerns and changes to the appearance that result from cancer treatment. We demonstrate a skincare routine to assist with side effects like dryness and sun sensitivity. We also provide makeup tips to help correct and conceal redness, sallowness, pigmentation, and dark circles, as well as techniques for drawing on eyebrows and eyelashes. Additionally, we offer advice on headwear options, including scarf styling and wig selection.
Even better, you walk away with a Confidence Kit full of skincare and make-up products donated by the cosmetic industry. Click here to register for a workshop.
Eyebrows: If you have time to get your eyebrows microbladed before your chemotherapy treatment, do it! Losing eyebrows during chemo can be emotionally challenging. Having microbladed brows can make the hair loss less noticeable and ease some of that stress. I lost all my eyebrows, but fortunately, I had already had my eyebrows tattooed a few months before my diagnosis. And they look very natural! I highly recommend Aesthetic by Reese in Pymble, who does an incredible job.
This is an excellent group gift idea for friends who want to give you something useful but don’t know what to buy.

Microbladed eyebrows still provide the structure to the face if you lose the hair in your eyebrows
9. Choose cleaner skincare products
I never paid much attention to the ingredients in my skincare until my breast cancer diagnosis. Now, it’s a priority. Many products contain endocrine disruptors and harmful chemicals that can be absorbed into the bloodstream. I’ve cleared out my old products and now only use clean skincare. I rely on the Yuka app, which scans barcodes and rates products out of 100, suggesting safer alternatives if needed. It’s been a game changer! Ingredients I avoid include parabens, phthalates, sulphates, artificial fragrances, and certain chemical sunscreens.
10. Take one day at a time
Some days during chemotherapy, you might feel terrible. Other days, you might feel surprisingly okay. Try not to let the thought of the entire treatment overwhelm you.
I found it helpful to focus on counting down each cycle. I kept track of how many I’d completed and how many were left. Each time I finished a cycle, it felt like a small victory, bringing me one step closer to the end.
It’s hard to imagine reaching that final day of treatment, but you will. One day, this challenging chapter will be behind you, and you’ll look back with pride at your strength and resilience. Keep going, take it one step at a time, and remember: you are stronger than you know.